Team
- Ahmad Abdal Qader
- Anapaula Avila
- Hamza Hasan
- Luis Borja
Customer
Dr. Ramzi El Hassan
Mentor
Laurel Carney
Problem Statement
Neck pain impacts 30% of adults in the United States. Prolonged poor posture is a direct cause of chronic neck pain. Poor posture is characterized as the rounding of the shoulders and forward protrusion of the head and neck, which strains the muscles and ligaments at the base of the cervical spine, resulting in neck pain[1]. Currently, there are devices in the market that attempt to address this issue, however, they detect movements that are not indicative of poor posture which does not provide a long-term solution to the problem at hand[2].
Approach and Objectives
With our device we aim to:
•Track the user’s posture by measuring the change in distance between their scapulae
•Notify the user during instances of poor posture
•Record and store the user’s postural data in a mobile application
In our approach we use the change in distance between the user’s scapulae as an indicator of a change in their postural position. With this approach we aim to build better habits in the user that improve their posture over time and prevent or ameliorate any neck pain that may arise from poor posture.
Device Hardware
To track the change in distance between the user’s scapulae we used a force sensitive resistor (FSR) and an elastic band anchored to the user’s shoulders.
The FSR and elastic band are coupled together using a spring embedded in a sponge attached to a plastic “buckle“. As the shoulders round, tension increases in the band and is translated into a focused compressive force onto the FSR.

To notify the user of their poor posture, we use a haptic motor that provides biofeedback in the form of a vibration.
Our main processing unit for our device is a Raspberry Pi which is responsible for raw data acquisition from the FSR, data analysis, and communication with the mobile app paired with our device.
Data Analysis
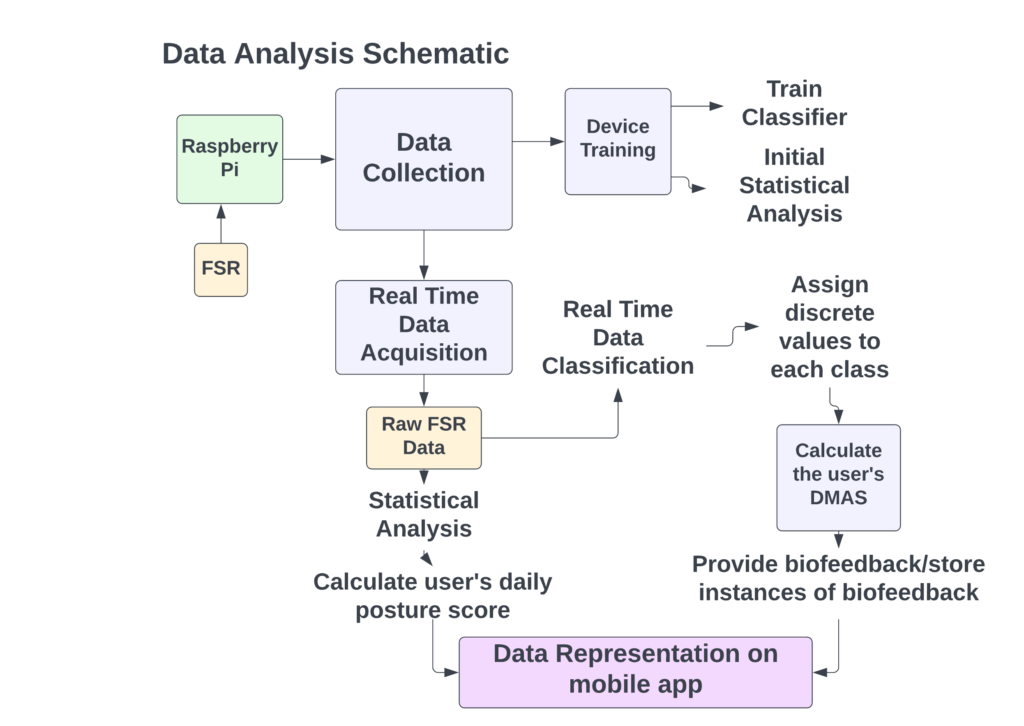
Figure 2 outlines our data analysis processes. Data is collected to train the device using a KNN classifier so that data can be classified in real time. The classified data is then assigned a discrete value based on its class label (Optimal-1, Suboptimal-2, Poor-3) and the sum of these values is taken over an 8-minute window of data acquisition. The value obtained is characterized as the user’s Discrete Moving Average Score (DMAS), whose magnitude dictates if biofeedback is triggered or not. The real time data is also analyzed to provide the user a Posture Score which represents the user’s daily posture status on a scale from 0-100 (0 – Poor Posture, 100 – Good Posture).
Testing
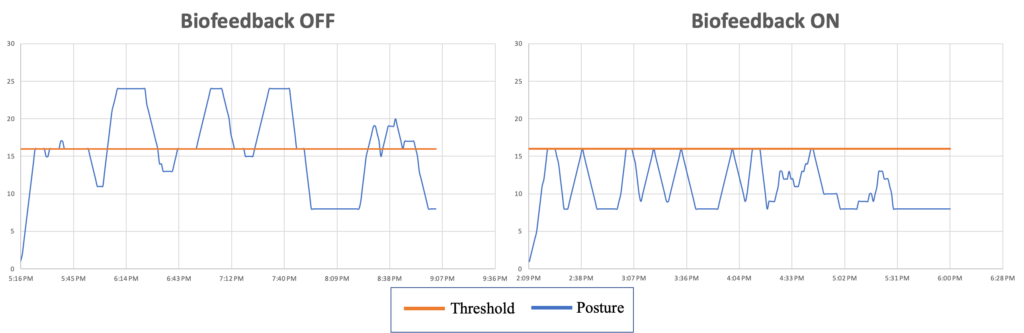
The figures above depict the user’s Discrete Moving Average Score (DMAS) over approximately a 4-hr period of desk activity. The threshold shown by the orange line represents the DMAS value at which biofeedback is activated to notify the user to correct their posture. In the left panel, the biofeedback functionality was disabled during data acquisition while the test user wore the device. In this scenario, the DMAS threshold was exceeded, and instances of poor posture were sustained for extended periods of time. In the right panel, the biofeedback functionality was enabled. It can be observed that the DMAS threshold was never exceeded, and posture was rapidly corrected after the user was notified. In the “Biofeedback On” case, after approximately 3 hours, the DMAS never reached the threshold to trigger a biofeedback event, potentially indicating a change in the user’s habitual posture patterns. This “Region of Awareness” is highlighted by the red bracket.
This test suggests that the device meets the intended use of improving postural habits in the user and alleviating the severity of postural positions that can lead to degenerative adaptations and cause neck pain.
Final Device
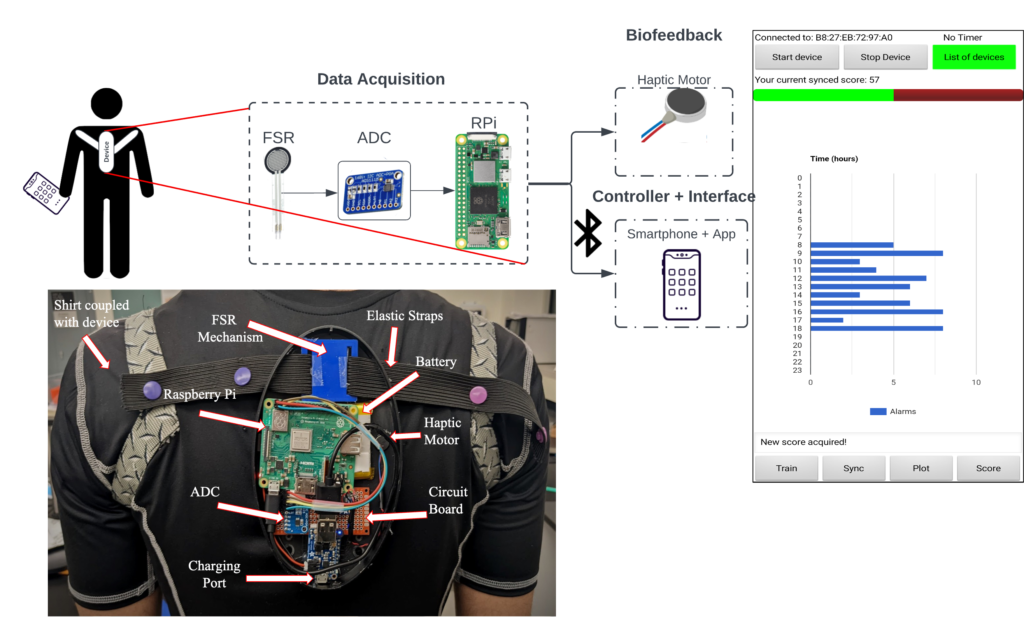
Conclusion/Future Work
The Cervical Spine Diary can accurately track scapular movements indicative of poor posture and notify the user during poor posture using haptic vibrations. The use of this device can be concluded to be an effective approach to preventing poor posture and building better postural habits in the user.
Future improvements involve miniaturizing the device and making the device independent of the shirt while maintaining accuracy of the data acquired. Additionally, the current estimated cost of the device is $159.30. Further emphasis can be placed on evaluating materials and production processes to lower down the product’s final price.
Acknowledgements
We would like to acknowledge Dr. El Hassan for providing us with this challenge and for his continued support throughout. We would also like to thank our supervisor, Dr. Carney for her guidance and expertise that greatly assisted in the development of this project. We would lastly like to thank our TA Mark Truskinovsky for his help throughout this process.
References
1. Cramer, H., Mehling, W. E., Saha, F. J., Dobos, G., & Lauche, R. (2018). Postural awareness and its relation to pain: Validation of an innovative instrument measuring awareness of body posture in patients with chronic pain. BMC Musculoskeletal Disorders, 19, 109. https://doi.org/10.1186/s12891-018-2031-9
2. Yoong, N. K. M., Perring, J., & Mobbs, R. J. (2019). Commercial Postural Devices: A Review. Sensors (Basel, Switzerland), 19(23), 5128. https://doi.org/10.3390/s19235128
